Obesity in the developing countries and around the world is an emerging public health threat with epidemic proportions. Widely accepted measure of obesity is body mass index (BMI). A ratio of weight (Kg) to height (m2). Normal range of BMI is considered 18.5 Kg/m2 to 24.9 Kg/m2. BMI of 30 and above is considered obese. This is further classified into class I, II, III obesity.

Bariatric surgery involves changing parts of the digestive system especially stomach and small intestines to help with weight loss where exercise and diet have not been effective. #Bariatric surgery becomes urgent if there are serious obesity-associated health concerns especially diabetes, hypertension, impending stroke, non-alcoholic fatty liver disease, sleep apnoea (breathlessness).
Who are the candidates of this surgery?
a) BMI of 40 (class III obesity) and above with no complications
b) BMI of 35 to 39.9 (class II obesity) and with weight related health complications such as type 2 diabetes, hypertension and sleep apnoea.

You need a screening process to see if you qualify for this surgery. You should be prepared to make the necessary changes to a healthier lifestyle. Participation in long-term follow-up plans that include monitoring your nutrition, lifestyle, behaviour and medical conditions if any is key for success.
Get in touch and book your screening appointment with our team.
What should you expect?
Most procedures limit amount of food. Others reduce the body’s ability to absorb nutrients while the remainder do both.
While weight loss surgery is beneficial, it is major surgery with potential for risks and side effects. Long term success of the surgery requires permanent healthy changes to diet and exercise.

Some of the risks involved include:
Immediate and short term:
v Excessive bleeding
v Infection
v Adverse reactions to anaesthesia
v Blood clot
v Breathing problems
Long term complications vary depending on type of surgery.
v Bowel (intestinal) obstruction
v Dumping syndrome that causes diarrhoea, flushing, nausea, light-headedness
v Micronutrient deficiencies
v Acid reflux
v Gallstones (some procedures)
v Hypoglycaemia
v Need for revision surgery.
How should you prepare for weigh loss surgery?
Upon qualifying for surgery, the team gives you instructions on how to prepare for surgery including different exams and lab tests to be done. You may have restrictions on eating and drinking before the surgery besides planning ahead for your recovery.
Weight loss surgery
Bariatric surgery is done under general anaesthesia. Some surgeries are done through traditional large open abdominal incisions. This surgery is cheaper, however, has longer recovery periods and is likely to have more complications.
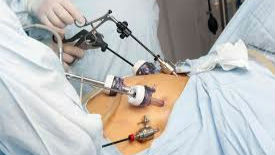
Most types of bariatric surgery are done laparoscopically. A laparoscope is a small tubular instrument with a camera attached. Small incisions are made on the abdomen where the laparoscope is inserted. The tiny camera on the tip of the laparoscope allows the surgeon to see and operate inside the abdomen without making traditional large incisions. This laparoscopic technique is increasingly available in most developing countries although more expensive than traditional abdominal surgery.
Surgery takes a few hours (average 2-4 hrs. It could be more depending on surgery).
After surgery you may stay in the recovery room as you awaken from the anaesthesia while being monitored for any immediate complications. Depending on procedure you may stay a few days in the hospital after surgery 2-3 days.
Types of bariatric surgery.
3 here are irreversible.
Gastric bypass
Sleeve gastrectomy
Duodenal switch and biliopancreatic diversion
Modified gastric fundoplication (Reversible)
More details about these procedures here:
In conclusion, the type of surgery you choose depends on your individual situation.
Bariatric surgery provides definitive long-term weight loss. https://www.bidahealthcare.com/
Bariatric surgery may fail long-term if you don’t follow recommended lifestyle changes, healthy diet and exercise.